Low-Dose Radiation Therapy: A New COVID-19 Treatment



This article is part of our series on radiation therapy. It describes an experimental treatment for COVID-19 that uses low-dose radiation techniques, discusses the possibility of treating patients with lung inflammation, describes the advantages of these techniques and efficiency for patient treatment, and discusses the results of the irradiation treatment in different laboratories around the world.
Introduction
Before antibiotics became a readily available and mainstream treatment option, American doctors used low-dose radiation with some success to treat pneumonia caused by bacteria or viruses. Now, this use of radiation therapy—specifically irradiating the patient’s lungs—is being revived, re-envisioned, and tested as a treatment for COVID-19 patients. In fact, experts and professionals in radiotherapy suggested this as a form of treatment during the first wave of the novel coronavirus outbreak, and now the first studies are showing promising results, with a consensus that low doses are well-tolerated.
COVID-19 and Its Effects
COVID-19 has a range of different symptoms and complications, including simple pneumonia. Pneumonia is an infection which causes the lungs to become inflamed and filled with fluid. When the air sacs in the lungs become filled with fluid, they are less able to take in oxygen, resulting in shortness of breath, cough, and other symptoms. COVID-19 can also lead to acute respiratory distress syndrome (ARDS), a form of lung failure. Patients with ARDS may need a ventilator to circulate oxygen in their bodies, as they are often unable to breath on their own.
Severe cases of COVID-19 can also result in sepsis, a serious condition that occurs when an infection spreads to and through the bloodstream, causing tissue damage all along the way. Sepsis can cause entire organ systems to shut down, including the lungs and heart. Even if a patient survives sepsis, they may have lasting damage to their organs, including the lungs.
Because the immune systems of patients with COVID-19 are preoccupied with fighting the virus, patients may be vulnerable to other infections in addition to the coronavirus. Panagis Galiatsatos, M.D., M.H.S., an expert on lung disease at Johns Hopkins Bayview Medical Center, explains that this can result in a “superinfection” that can, in turn, increase damage to the patient’s lungs.
Low-Dose Irradiation and COVID-19
The use of radiotherapy to treat pneumonia dates back to the early part of the 20th century, when American publications describe that very low-dose irradiation of the lungs made it possible to quickly cure certain patients who had bacterial or viral infections. At the time, doctors did not have a computed tomography, but by doing X-rays and monitoring the patient’s temperature, they found that patients’ condition improved within 6 to 8 hours. Patients were no longer feverish, and they seemed well on the road to recovery.
At the beginning of the COVID-19 pandemic, researchers and radiotherapist oncologists in different parts of the world considered reviving this old idea and putting it to new use. Some were skeptical, warning that irradiating the lungs of people infected with the novel coronavirus could trigger immunosuppression that would promote the outbreak of the virus. Others argued that there simply was not enough evidence to support experimenting with this treatment, and the risks to participants in the proposed studies was too great. Others argued that there was enough evidence to warrant further trials. The difficulty was that they did not know what dose to test. At the time this treatment was originally developed, everything was very different in the way radiotherapy was done, including the prescription of the dose, the X-rays used, even how experiments were conducted and data collected.
Ultimately, and perhaps not in a little desperation, new studies inspired by the old technique were initiated, experimenting with low-dose irradiation as treatment for COVID-19. Some of these initial studies have since found that low-dose radiotherapy can improve the condition of patients with pneumonia caused by COVID-19. In some severe COVID-19 cases, especially those in which patients develop severe lung conditions, low-dose radiation also appears to be beneficial.
Materials and methods

Several small-scale studies with varying approaches have been launched around the world. One approach was to use clinical trials with small numbers of patients in which patients were treated using a linear accelerator. Doctors then monitored patients’ conditions and toxicity. Another approach was to better understand what was happening to patients’ lungs using a model of pneumonia in mice.
This consists of placing products in the trachea of mice which mimic a microbial or viral infection, visible on the scanner; researchers then showed that low doses of irradiation inhibited pneumorrhagia. Most importantly, low dose radiation was found to be effective at a dose of 0.5 Gray. For comparison, radiation therapy for lung cancer is delivered at a dose of 66 Gray in 33 fractions, so the dose in COVID-19 treatment is 132 times lower than in cancer treatment.
Results and discussions
Physicists have characterized an immunological subpopulation, peri nervous macrophages, which are reprogrammed by irradiation. Macrophages are inflammatory cells that secrete cytokines that either have an anti-inflammatory (interleukin 10) or pro-inflammatory (interleukin 6) effect. Irradiation reprograms macrophages to an anti-inflammatory phenotype, stimulating the secretion of interleukin 10 and inhibiting that of interleukin 6.
Based on this understanding, researchers treated fragments of human lungs with low-dose radiation, achieving positive results. Oncologists wanted to see the effect on real viruses, but at the time of the first COVID-19 wave, they did not have easy access to the COVID-19 virus. So doctors worked with the pandemic H1N1 virus which induces severe pneumonia in mice and humans. Similarly, physicists have observed that low dose irradiation induces an anti-inflammatory profile of macrophages.
It is expected that doctors will soon receive the authorizations to conduct the same experiments with the actual COVID-19 virus, SARS-CoV-2; for this, they are working in different Laboratories around the world, primarily in the United States of America, France, Iran, Spain and India.
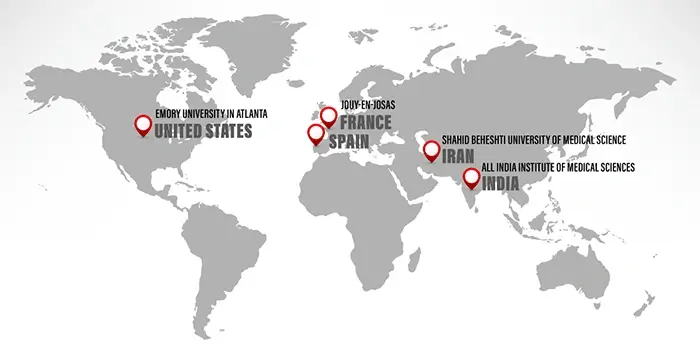
A US team from Emory University in Atlanta, Georgia has released the data from their first trial in which they treated COVID-19 patients with a slightly higher dose (1.5 Gray). Researchers in this trial concluded that there is no risk of worsening the patient’s condition and patients benefit from rapid improvement, findings similar to those in the previously mentioned historical studies. Though the study was small, the results are promising, so much so that the researchers will conduct a randomized study.
A team from Shahid Beheshti University of Medical Sciences in Tehran, Iran published their findings in the American journal International Journal of Radiation Oncology, Biology, Physics. The authors concluded that using low-dose radiation to treat COVID-19 patients was feasible.
At the end of November, a team from Madrid released the preliminary report of a small study in which COVID-19 patients were treated with doses of 0.7 Gray. The results were positive. The team concluded that low-dose radiation was a feasible treatment for COVID-19 patients.The authors of the report also noted that the doses were well-tolerated by patients and could potentially improve patients’ conditions.
Additionally, a team of researchers from the All-India Institute of Medical Sciences in New Delhi, India have just released similarly encouraging results from a small study of COVID-19 patients, in which almost all patients recovered within 3-7 days after receiving low-dose radiation treatment.
These studies are contributing to a growing body of evidence that low doses of radiation are well-tolerated by COVID-19 patients; that there is no major radiation-induced worsening in patients’ conditions, and that there are many patients whose conditions improve after treatment. Of course, it remains to be proven through randomized clinical trials (for which many of the previously mentioned studies call in their concluding remarks) whether this is effective for patients. The efficacy of this experimental treatment for COVID-19 is the subject of ongoing studies in progress after these reassuring preliminary studies.
Final Thoughts
Even with the positive results coming in from these initial studies of low dose radiation to treat COVID-19 patients, it is important to bear in mind that even these low doses of radiation can have carcinogenic effects. However, what we know today from multiple studies is that it takes between 10 and 15 years to (potentially) induce cancer at doses so low. So the question then becomes, do you refuse to use potentially life-saving treatment to someone who has a life expectancy of less than three weeks to avoid the increased risk of developing cancer in 10 to 15 years, especially if the patient is elderly and presents with comorbidities? What if the patient is young? Ethics committees and physicians will surely be grappling with this question as trials move forward in more places and the world marks more than 2 million deaths while it witnesses a new, horrifying rise in the numbers of cases.