The Evolving Role of Radiation Therapists



- Introduction – an overview of how the role is expanding; outpatient, education, and non-traditional settings
- Increased responsibilities – in the clinic, with new technology, adaptive treatment planning, and supportive care.
- Professional Development – more involvement in peer mentoring, onboarding, supporting students and new graduates, involvement in professional societies, and advocacy for the profession.
- Multidisciplinary collaboration – working physicians, nurses, specialists, dosimetrists, and physicists to improve workflow and outcomes.
- New Technology – Learning advanced systems, new imaging, and AI integration in radiation therapy.
- Expanded Pathways – options in radiation therapists’ career pathways and non-traditional roles (i.e., dermatological, education, clinical application specialist, veterinary, proton therapy, MR, etc.)
- Conclusion – final thoughts on the future direction of the profession and how to support these evolving roles in our profession.
Introduction
When I first entered the profession, my focus was clear: deliver safe, precise treatments. Learn the machine. Follow protocol. Protect the patient. And that all still matters.
But over the years, I’ve watched our role expand. Not away from precision but beyond it. Radiation Therapists are more visible in clinical conversations, more involved in education and advocacy, and more integrated in the patient experience than many people outside our field realize. And we’re still evolving.
If you graduated ten years ago, the job probably feels different today. If you graduated twenty years ago, it feels very different. The role of the Radiation Therapist is growing, not just in technology, but in responsibility, leadership, and opportunity!
From outpatient oncology and dermatologic settings to education and advanced practice conversations, Radiation Therapists are moving into spaces that used to fall outside the traditional path.
Our profession is being refined, and that refinement is creating more opportunities than ever.
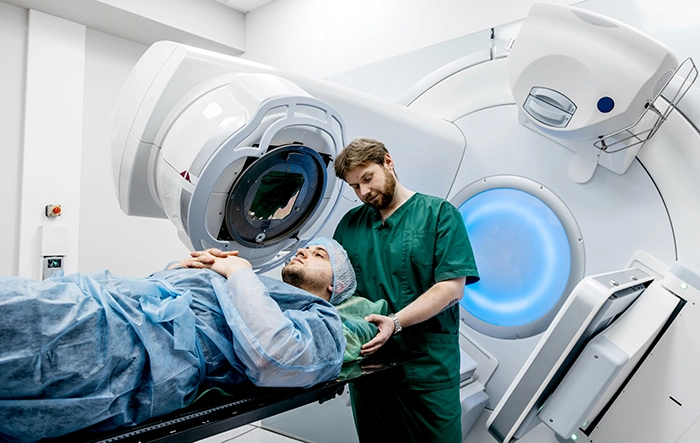
Increased Responsibilities in the Clinic
At its core, radiation therapy is still about safe, accurate treatment delivery and compassionate patient care. Our foundation has not changed. What has changed is how much more we’re trusted to see, evaluate, and contribute.
We’ve all heard the outdated phrase “button pushers.” Most of us hate it. Anyone who has worked on a busy linac and caught a setup discrepancy before it became a problem knows this job is anything but passive.
Radiation Therapists assess patient needs, review daily imaging, recognize subtle anatomical shifts, escalate concerns, and collaborate thoughtfully in real time. Adaptive workflows and high-tech imaging systems have not minimized our role. They’ve expanded it.
But here’s what technology will never replace: our bond with our patients.
In many departments, Radiation Therapists naturally take on supportive care responsibilities. We monitor side effects. We explain what to expect. We coordinate care with the multidisciplinary team. All while being a steady presence for patients every single day. For many patients, the Radiation Therapist is the most consistent member of their treatment team, and our consistency creates trust.

We notice when a patient seems quieter than usual. We recognize changes before they are verbalized. Artificial intelligence (AI) can optimize our workflows, but it cannot sit beside a patient who is overwhelmed and hold their hand. It cannot replace the relationship we built over those weeks of treatment.
If anything, evolving technology should allow us to focus even more on what matters most: caring for patients and upholding the passion and commitment that define our profession.
Professional Development and Mentorship
The evolution of our role reaches beyond the treatment room.
Mentorship and onboarding have always been part of what builds strong departments. Experienced Radiation Therapists guide new graduates through their first year, helping them turn their classroom knowledge into clinical confidence. That support strengthens safety culture and strengthens teamwork.
Today, mentorship may feel more complex. Generational differences in communication styles and expectations can create tension or misunderstanding. That does not make mentorship less important; it simply means it calls for intention. Our profession is strongest when experience and fresh perspective work together.

At the same time, conversations about Advanced Practice Radiation Therapists are gaining traction. These discussions bring excitement and, understandably, questions about boundaries and collaboration. That’s healthy. It means we care about our scope of practice and our patients.
Growth does not need to divide us. Advanced roles should improve team function, not replace it. If we are grounded in the principle of prioritizing patient care, every advancement forward will strengthen our profession.
Multidisciplinary Collaboration
Radiation Oncology has always been collaborative, but Radiation Therapists’ voices are becoming a larger part of conversations both inside and outside the clinic.
Within our departments, we work closely with physicians, nurses, dosimetrists, physicists, and members of the care team to improve workflows and clinical outcomes. We are often the bridge between treatment planning and delivery. We see how decisions translate from a treatment plan to the individual on our treatment table, and our perspective is valuable.
Collaboration also goes beyond the clinic. Radiation Therapists who engage in professional organizations, such as the American Society of Radiologic Technologists (ASRT) or their state affiliate societies, help shape the standards, policies, and advocacy efforts that influence our daily practice. Our active role in these organizations strengthens our unified voice and assures that Radiation Therapy remains visible in wider discussions.
Equipment improves when we provide feedback. Education evolves when we share real-world experience. Scopes of practice and standards of care are protected when professionals stay involved. Progress in our profession does not happen by accident. It happens when Radiation Therapists choose to engage at the local, state, and national levels, as well as within their own departments.
Technology, AI, and Responsibility
There is no denying that technology is advancing rapidly. AI-assisted tools, automated contouring, and integrated platforms are becoming part of everyday practice.
These systems offer real advantages, including improved consistency, added safety checks, and workflow efficiency. They can reduce manual burden and allow Radiation Therapists to redirect energy toward patient interactions. But technology does not eliminate responsibility.
If history in healthcare has taught us anything, it is that what appears on a screen is not a substitute for professional judgment. Machines are powerful, but they are not flawless. Radiation therapy has always depended on layers of safety systems and alert clinicians. That does not change in an AI-supported environment.
AI should support our expertise in radiation therapy, not replace it. Automation should strengthen safety culture, not create complacency. So, if integrated thoughtfully, innovation allows Radiation Therapists to do what we already do well… only better.
Radiation Therapists’ Expanded Career Pathways
Another exciting development is the expansion of career pathways available for Radiation Therapists.
Traditional hospital-based roles are still foundational, but Radiation Therapists are also practicing in outpatient oncology centers, dermatology offices, proton therapy centers, MR-guided environments, veterinary offices, education, research, and clinical applications roles.
This flexibility supports longevity in the profession and gives Radiation Therapists the freedom to find the environment where they do their best work. Some are drawn to fast-paced, high-intensity settings. Others prefer travel opportunities or more adaptable schedules. For some, stability and family-centered routines matter most. Many step into mentorship, leadership, or technology-focused roles as radiation therapists’ careers evolve.

These shifts are not about stepping away from the profession, and no path carries more value than another. Each role contributes to the same common mission of enhancing outcomes and advancing cancer care. A profession with different pathways keeps talented Radiation Therapists engaged, supports long-term careers, and sustains the passion that brought many of us here in the first place.
Looking Ahead
The role of the Radiation Therapist is not expanding because it is trendy. It is expanding because patient care is more complex, technology is more sophisticated, and healthcare calls for more collaboration than ever before.
That growth requires Radiation Therapists who are clinically sharp, adaptable, and engaged in the direction of the profession. It also requires us to be grounded in what has always defined this work.
Radiation therapy has never been just about machines. It has always been about responsibility. It has always been about precision paired with compassion and professionals who understand that the person on the table is not a treatment plan, but a human being placing trust in us.
The technology we use will continue to evolve, our systems will change, and our career pathways will expand. What should always remain constant is the standard we hold ourselves to.
The future of radiation therapy will not be defined solely by technology. It will be defined by the people behind it. By professionals who remain curious, accountable, and committed to patient care. The evolution of our profession is not something ahead of us; it is already here, and we are the ones shaping it.
Disclaimer: The information provided on this website is intended to provide useful information to radiologic technologists. This information should not replace information provided by state, federal, or professional regulatory and authoritative bodies in the radiological technology industry. While Medical Professionals strives to always provide up-to-date and accurate information, laws, regulations, statutes, rules, and requirements may vary from one state to another and may change. Use of this information is entirely voluntary, and users should always refer to official regulatory bodies before acting on information. Users assume the entire risk as to the results of using the information provided, and in no event shall Medical Professionals be held liable for any direct, consequential, incidental or indirect damages suffered in the course of using the information provided. Medical Professionals hereby disclaims any responsibility for the consequences of any action(s) taken by any user as a result of using the information provided. Users hereby agree not to take action against, or seek to hold, or hold liable, Medical Professionals for the user’s use of the information provided.

