Skeletal Trauma and Child Abuse in Pediatric Imaging

Skeletal Trauma and Child Abuse in Pediatric Imaging
A review of children’s bone anatomy, the fracture patterns common and unique to children, and the potential signs of child abuse in pediatric trauma cases


It is important for you as an RT to be aware that in the course of imaging children in your daily work, you could be creating significant evidential documentation related to nonaccidental injuries (NAI). If the child you are imaging is suspected of having received these injuries from physical abuse, you may be called upon later to participate in legal proceedings. If you are unaware of child-protection procedures, you could unintentionally place the child and yourself in jeopardy through seemingly simple actions such as questioning the child. Also, if you fail to report the case, it has major implications for any legal proceedings. For the wellbeing of the child, it is important that you stay informed about what to look for and what you should and should not do in such cases.
In this article, we will review pediatric classifications and age ranges, parts of bone growth on radiographs, and different types of pediatric skeletal trauma, along with identifying potential signs of child abuse that you should be on alert for. We’ll also address your role and obligations as a radiologic technologist in cases of suspected child abuse.
- A Quick Definition of Pediatrics
- Pediatric Bone Growth and Structures
- Common Types of Pediatric Trauma
- CT in Pediatric Trauma Imaging
- Pediatric Skeletal Trauma and Signs of Child Abuse
- Potential Signs of Abuse in Children with Fractures
- Skeletal Surveys
- Your Duty to Report
A Quick Definition of Pediatrics
Pediatrics is medical practice that provides healthcare to infants, children, and adolescents. According to the The American Academy of Pediatrics (AAP), anyone under the age of 21 should receive pediatric medical care, because children are not just smaller adults—they have specific and special developmental and health needs that differ from those of adults. The table below provides a break down of different pediatric classifications and their age ranges.
| Name | Defintion |
| Neonates | Newborns up to one month |
| Infants | One month to two years |
| Children | Two years to twelve years |
| Adolescents | Twelve years to sixteen years |
| Pre-Adults | Sixteen years to twenty-one years |
Pediatric Bone Growth and Structures
Pediatric bones are more porous and less well mineralized than adult bones, and, as a result, are softer than adult bones. Pediatric and adult bones distinctly different anatomically, and specific system for identifying and naming different pediatric fractures and the affected regions of the pediatric bone.
Pediatric bones have a physis or growth plate. This growth plate appears as a lucency between the flared metaphyseal region of the bone and the growth center (epiphysis). The shaft is called the diaphysis. Children’s bones grow in length through endochondral ossification at the metaphyseal edge and also in width.
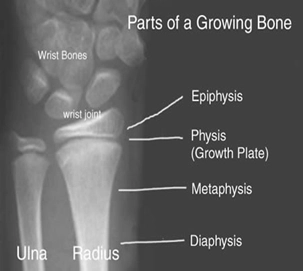
Source: [LINK]
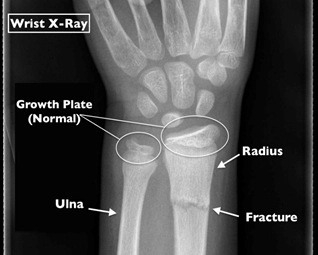
Source: [LINK]
The gist: The bones of children and adults have marked differences in anatomy, and you should familiarize yourself with the special terminology used for classifying pediatric fractures.
Factors That Influence Pediatric Peak Bone Mass
- Gender: Males have a higher bone mass (or bone density) than females. Boys and girls develop bone mass at similar rates before the onset of puberty, and after puberty, boys typically gain more bone mass than girls.
- Race: We really don’t understand why, but female African Americans tend to have a higher peak bone mass and are at a lower risk for osteoporosis in their later years than are white females. We still need more research to better understand the role of race and ethnic groups in differences in bone density. However, because all women of any and all races are at significant risk for osteoporosis, all girls need to build as much bone as possible in an effort to protect themselves from the disease.
- Hormonal factors: Estrogen and testosterone are essential in developing bone mass. Girls who begin menstruation at a younger age tend to have greater bone density. Those girls whose period are irregular (those who often miss menstrual periods) can sometimes have lower bone density.
- Nutritional status: Calcium is vital for bone development and health, along with a well-balanced diet the includes sufficient vitamins and minerals, such as magnesium, zinc, and vitamin D.
- Physical activity: Physical activity is important for building healthy bones. Children should be encouraged to exercise, run, and play sports and avoid sitting all day. Being physically active is most beneficial for the parts of the skeleton that bear the brunt of a child’s weight, such as the hips and the arms (when lifting/carrying things).
The gist: Many factors affect a child’s peak bone mass, some of which we can influence (e.g., nutrition) and some which are fixed (such as biological gender).
Common Types of Pediatric Trauma
Children’s fractures tend to be different from those of adults. In pediatric trauma, we see fracture patterns related to age. Infants tend toward diaphyseal fractures, children toward metaphyseal fractures, and adolescents toward epiphyseal fractures.
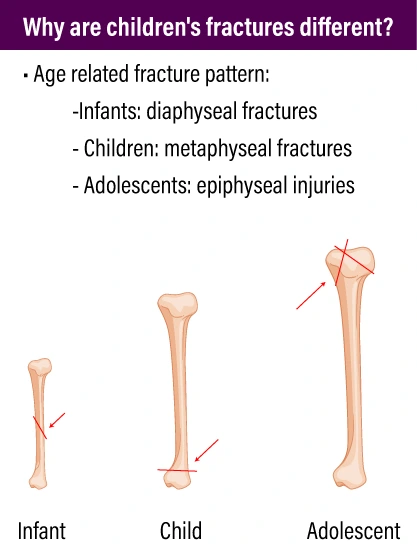
Types of Common Pediatric Fractures
There are many types of fractures, some more common in children than others. And some fracture patterns seen in pediatric trauma are utterly unique to the pediatric population.
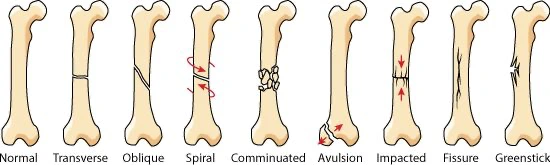
Three common fracture types in children are (1) the plastic deformity, (2) the “buckle” or torus fracture, and (3) the greenstick fracture.
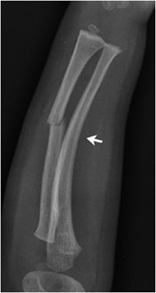
Fig. 1 – Source: [LINK]
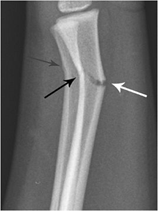
Fig. 2 – Source: [LINK]
A plastic deformity fracture is a bone that has bent without a visible fracture line. There are likely microscopic fractures on the concave or compression side of the injury. These types of fractures are often seen in the forearm or lower leg where two bones are present. Figure 1 (right) shows a radiograph of a frontal forearm with a plastic deformity (bowing) of the ulna with excessive radial curvature of the shaft (arrow). Incident note made of midshaft radial fracture. The ulna and fibula are commonly affected, and there may be a complete fracture of the other paired long bone. Radiographic findings may be so subtle that it is not unusual to see the fracture deformity only after callus formation is identified.
A greenstick fracture is a unicortical fracture, in which only the bent side of the is cortex interrupted. This is more common in children. In adults, the fracture tends to penetrate both cortices. Figure 2 (right) shows a lateral forearm radiograph with a unicortical greenstick fracture of distal radial diametaphyseal region (white arrow), plastic deformity of dorsal cortex at the same level (thick black arrow), and small buckle fracture diametaphyseal region of ulna (thin black arrow).
The Salter-Harris Skeletal Fracture Classification System
Epiphyseal injuries usually involve the physis (growth plate) and so are often the source deformities in a healed fracture. To describe fractures in the physis, epiphysis, or metaphyseal margin of the bone adjacent to the the physis, the Salter–Harris classification system is used, developed by Salter and Harris in 1963. The system is simple and is the most widely used classification system. It describes five types of growth plate injuries classified according to medical imaging findings in the epiphysis, physis, and metaphysis. While a physis injury may not be visible on the scanned image, it is assumed that injury is propagated into the growth plate.
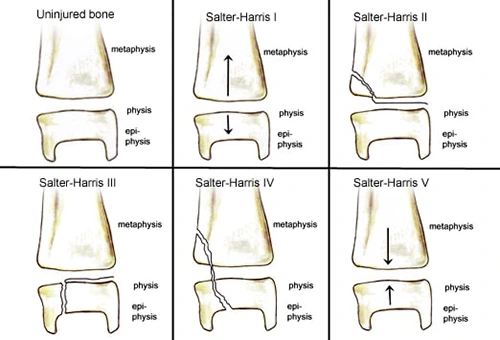
Salter fractures can have long-term complications that include differences in the lengths of limbs and joint incongruity.
Figure 3 (right) is a radiograph of a lateral ankle showing a Salter IV fracture of the distal tibia. The fracture line intersects the metaphysis (arrowhead) and the epiphysis (arrow) with some posterior displacement of both fracture fragments. Additional fibular diaphyseal and medial malleolar fractures are also present.
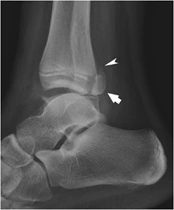
Fig. 3 – Source: [LINK]
A Salter IV injury is intra-articular and involves both the epiphysis and metaphysis. This type of fracture carries with it a risk of premature fusion of the physis, which can cause an angular deformity around the joint, or incongruity of the articular surface.
Pediatric Head Trauma
Head injuries are among the most common causes of disability and death in children. Common causes of head injuries are sports, a fall, car accidents (including when a child is a passenger in the vehicle at the time of the accident and when a child is hit by a car). Child abuse and shaken baby syndrome are also among the causes pediatric head trauma.
The below image shows an 8-year-old child who fell from a bike. Initial non-contrast head CT shows a left epidural hemorrhage (A). Follow-up rMRI axial T2 shows interval-increased size of the left epidural hemorrhage (B). Follow-up rMRI axial T2 TSE shows craniotomy and evacuation of the left epidural hemorrhage (C).
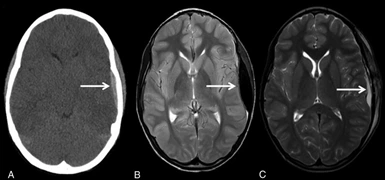
Source: [LINK]
- A concussion is a head injury that can cause immediate loss of alertness for anywhere from a few minutes to a few hours
- A contusion is a bruise on brain that causes bleeding and swelling.
- A skull fracture is a break in the bones of the skull. There are 4 major types of skull fractures: linear, depressed, basilar, and diastatic
The diagnosis of a head injury may include diagnostic radiographs, MRI, or CT scans. Though X-ray exams are helpful in diagnosing skull fractures, A CT scan can detect most skull fractures as well as produce images of the brain. So, if a brain injury is suspected, a CT scan alone may be used to reduce the radiation dose to the patient.
The gist: The four distinct types of skull fractures can cause concussions, contusions, or brain bleeds. While most fractures are a result of accidental trauma, non-accidental injuries can occur as a result of child abuse.
Pediatric Torso Trauma
Blunt trauma is a type of skeletal trauma that occurs when the body is hit by a heavy object with great force. When injuries occur to the skeletal muscles, this also is a type of skeletal trauma, typically classified as a musculoskeletal injury.
There were 110,525 cases of pediatric blunt torso trauma in the United States in 2016. However, the prevalence of intra-abdominal injury (IAI) has been found to be as low as 6.3%. And, of those IAI cases, less than 2% required an intervention.
The gist: While blunt pediatric abdominal trauma occurs frequently, the number of IAI that require medical intervention is low.
CT in Pediatric Trauma Imaging
Non-pediatric level 1 trauma centers tend to use computed tomography (CT) for evaluating pediatric trauma patients more often than pediatric trauma centers do, even when you account for the severity of the injury. CT is superior to other imaging modalities in identifying penetrating trauma injuries, but the radiation exposure that comes with it means CT should used with caution for child patients (check out our Reducing Radiation Dose in Pediatric CT course for more information on the subject). CT should be used for patients receiving nonoperative care because they are effective at screening for peritoneal penetration.
The image below shows a computed tomogram of the abdomen and pelvis of a four-year-old boy showing a small, thin foreign object in the left upper quadrant (indicated by the white arrow) (A). The sagittal view (B) suggested a potential penetrating bowel injury by a foreign body, which was not detected by physical examination.
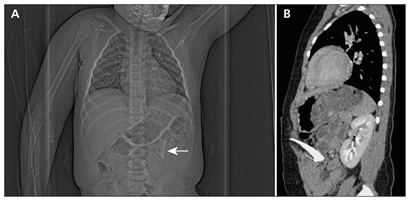
Pediatric Skeletal Trauma and Signs of Child Abuse
Child abuse is an act (or a failure to act) that results in harm or the potential or threat of harm to a child, typically done by an adult with authority over the child. It is non-accidental in nature, and can be the result of a deliberate intention to cause the child harm, or the result of knowingly reckless or careless behavior that put the child in danger and resulted in injury. The radiology department is one of the first points of contact and plays a vital role in the detection of physical abuse. For any child coming in with such injuries, abuse should always be part of the diagnostic consideration considering how serious the consequences are for that child if the abuse goes undetected. Simple X-rays, often skeletal surveys, are the best indicator of a child’s injuries, both past and present. In cases of suspected abuse, a highly skilled radiographer is charged with acquiring the best diagnostic images possible to assist in this diagnosis. If this task falls to you, it is their duty to call the radiologist’s attention to pathologies you see on the images.
While fractures are common in pediatric patients, with most being from falls and various forms of accidental trauma, a significant number of abused children present with head and skeletal trauma. Younger children are more likely to have fractures resulting from abuse. As children get older, they are more likely to have accidental fractures. Fractures are found in 11% to 30% of infants and children who are evaluated for possible physical abuse. But because pediatric fractures are common, those that are the result of abuse can go unrecognized as such, particularly in infants and young children. However, we can identify the features of the fracture that suggest the injury is non-accidental.
Potential Signs of Abuse in Children with Fractures
There are several warning signs that may indicate child abuse that you should be aware of whenever you are imaging a pediatric skeletal trauma. These can be in the patient history of the child and/or they can be clinical in nature.
- There is no history of trauma, or the injury was unwitnessed
- The child’s history is incompatible with their age/developmental stage OR with the injury
- The history changes with repeated retellings
- The was a delay in seeking medical attention
- The child is less than 1 year old
- The child’s images show high-risk fractures:
- Rib fractures
- Metaphyseal fractures
- A humerus fracture in a child younger than 18 months
- A femur fracture in a child who is not yet walking
- Multiple fractures
- The child’s images show fractures of different ages
Other injuries, such as burns, bruises, and/or swelling, may also be signs of child abuse. Bear in mind children who are are too young to give their own clinical history or account of the trauma or who cannot do so because of cognitive or developmental delay require extra attention from you.
The gist: Though fractures are common in children, there are specific signs, both historical and clinical, that may indicate the child’s fracture was not the result of an accident, but of child abuse. You should familiarize yourself with this list, and be sure to draw the radiologist’s attention to any potential red flags you noticed.
Skeletal Surveys
A skeletal survey (SS) is the radiology department’s tool of choice investigating fractures with unclear causes. This is because a skeletal survey provides valuable information about the patient’s bone health and may identify skeletal injuries that have no immediately obvious or outward signs. Think back to your radiography educational program. You likely learned how important an SS is. It is vital that you review skeletal survey educational material often to keep it fresh in your mind. You are accountable for your practice, which must always promote and safeguard the well-being of children in their care. Knowing how to perform a flawless SS is part of that.
A skeletal survey is recommended for children under 2 years old when child abuse is suspected. Even though it is less likely to produce positive findings when the child is older than 2 years, a physician should consider imaging children up to 5 years of age if it is strongly suspected that the child may have injuries that are not readily discernible. The guidelines for appropriate pediatric skeletal survey pediatric imaging are laid out by the American College of Radiology (ACR) and endorsed by the American Academy of Pediatrics (AAP).
The below image shows multiple bilateral posterior rib fractures that are healing seen in an infant who also has an acute left clavicle fracture.
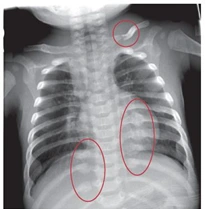
Source: [LINK]
Your Duty to Report
If a pediatric patient in your care presents with trauma that you suspect may be the result of child abuse, you have a duty—legal, ethical, professional, and personal—to report it. And because the specific letter of the law varies a bit from state to state and country to country, you must also be well-informed on how you must proceed in such a case to protect both the child and yourself. Dealing with these cases can be complex, and often they require a great deal of personal and interpersonal skills, knowledge of legal policy and child-protection procedures, and a good deal of emotional strength. Be sure to discuss and thoroughly understand your institution’s protocol for reporting suspected cases of child abuse with your supervisor or the institution’s legal team for specific guidance, as the legal requirements and consequences may vary from state to state. In such cases, keeping your knowledge up to date and ensuring you know procedure may directly save a child from continued suffering and may even save a life.
References
- American Academy of Pediatrics, Section of Radiology. (2009). Diagnostic imaging of child abuse. Pediatrics, 123(5), 1430–35.
- Belfer, R. A., Klein, B. L., & Orr, L. (2001). Use of the skeletal survey in the evaluation of child maltreatment. The American Journal of Emergency Medicine, 19(2), 122–124. [Link]
- Chauvin-Kimoff, L. Allard-Dansereau, C., Colbourn, M., & Canadian Paediatric Society, Child and Youth Maltreatment Section. (2018). The medical assessment of fractures in suspected child maltreatment: Infants and young children with skeletal injury. Paediatric Child Health, 23(2):156–160. [Link]
- Como, J. J., Bokhari, F., Chiu, W. C., Duane, T. M., Holevar, M. R., Tandoh, M. A., Ivatury, R. R., & Scalea, T. M. (2010). Practice management guidelines for selective nonoperative management of penetrating abdominal trauma. The Journal of Trauma, 68(3), 721–733. [Link]
- Davis, M. & Reeves, P. (2009). Diagnostic radiographers and their role in child protection situations-An exploration of bystander intervention. Child Abuse Review, 18(3), 205-214. [Link]
- Duffy, S. O., Squires, J., Fromkin, J. B., & Berger, R. P. (2011). Use of skeletal surveys to evaluate for physical abuse: analysis of 703 consecutive skeletal surveys. Pediatrics, 127(1), e47–e52. [Link]
- Fulton, L. (2017, November 20.). A basic understanding of the role of radiology in cases of suspected physical child abuse. Junglist. [Link]
- Head injury in children. (n.d.) Hopkins Medicine. [Link]
- Holmes, J. F., Lillis, K., Monroe, D., Borgialli, D., Kerrey, B. T., Mahajan, P., Adelgais, K., Ellison, A. M., Yen, K., Atabaki, S., Menaker, J., Bonsu, B., Quayle, K. S., Garcia, M., Rogers, A., Blumberg, S., Lee, L., Tunik, M., Kooistra, J., Kwok, M., … Pediatric Emergency Care Applied Research Network (PECARN) (2013). Identifying children at very low risk of clinically important blunt abdominal injuries. Annals of Emergency Medicine, 62(2), 107–116.e2. [Link]
- Marin, J. R., Wang, L., Winger, D. G., & Mannix, R. C. (2015). Variation in Computed Tomography Imaging for Pediatric Injury-Related Emergency Visits. The Journal of Pediatrics, 167(4), 897–904.e3. [Link]
- Mehta, H., Acharya, J., Mohan, A. L., Tobias, M. E., LeCompte, L., & Jeevan, D. (2016). Minimizing radiation exposure in evaluation of pediatric head trauma: Use of rapid MR imaging. American Journal of Neuroradiology, 37(1), 11–18. [Link]
- National Institutes of Health. (n.d.) Kids and their bones: A guide for parents. [Link]
- Skeletal trauma: General and unique considerations in children. (2017, January 10). Radiology Key. [Link]
- Swoboda, S. L., & Feldman, K. W. (2013). Skeletal trauma in child abuse. Pediatric annals, 42(11), 236–243. [Link]
- Wenokor, C. (2017, January 14). Pediatric skeletal trauma. Radiology Key. [Link]
Disclaimer: The information provided on this website is intended to provide useful information to radiologic technologists. This information should not replace information provided by state, federal, or professional regulatory and authoritative bodies in the radiological technology industry. While Medical Professionals strives to always provide up-to-date and accurate information, laws, regulations, statutes, rules, and requirements may vary from one state to another and may change. Use of this information is entirely voluntary, and users should always refer to official regulatory bodies before acting on information. Users assume the entire risk as to the results of using the information provided, and in no event shall Medical Professionals be held liable for any direct, consequential, incidental or indirect damages suffered in the course of using the information provided. Medical Professionals hereby disclaims any responsibility for the consequences of any action(s) taken by any user as a result of using the information provided. Users hereby agree not to take action against, or seek to hold, or hold liable, Medical Professionals for the user’s use of the information provided.
