Understanding Emotional Health: A Rad Tech’s Guide



Radiologic technologists, along with other healthcare professionals, have been bearing the weight of unprecedented challenges during the protracted COVID healthcare crisis. Now, with the new Omicron variant threatening to cause yet another surge of cases in a pandemic that has been ongoing for two years, and with vaccine uptake stagnating, it is again important for radiologic technologists to identify and address stress, fatigue, and burnout and their effects on emotional health.
Stress injuries can cause more than just burnout among rad techs and other healthcare professionals. Many of us still have not got the hang of dealing with the stressful situations that this health crisis has put us in. So, let’s take a look at stress, fatigue, burnout, and emotional health, what they are, how they differ, their effects, and some healthy ways to manage them.
- Differences in stress, fatigue, and burnout, and defining emotional health
- Stressors
- COVID-19’s Role in Radiologic Technologist Burnout
- Gender Differences
- Coping Mechanisms
- Final Thoughts
- References
Differences in stress, fatigue, and burnout, and defining emotional health
- Stress: We can define stress as a state of mental or emotional strain or tension resulting from adverse or very demanding circumstances. It can have serious effects on physical, emotional, and psychological health.
- Fatigue: Fatigue is the body’s signal that a rest period is needed. Long work hours and extended and irregular shifts may be stressful physically, mentally, and emotionally. Headaches, muscle tension, irritability, and high blood pressure are all symptoms of fatigue that can escalate and kill if stress is not dealt with. Remember, worker fatigue increases the risk for illnesses and injuries. In fact, studies have shown that accident and injury rates are 18% greater during evening shifts and 30% greater during night shifts when compared to day shifts.
- Burnout: Burnout is a long-term stress reaction marked by emotional exhaustion, depersonalization, and a lack of sense of personal accomplishment. Healthcare workers seem to be at particular risk for burnout, especially during these recent events.
-
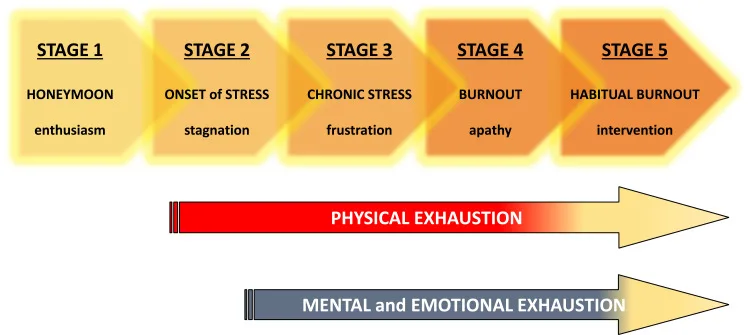 Simplified 5-stage model of development of burnout
Simplified 5-stage model of development of burnout - Emotional health: Emotional health, a concept synonymous with wellbeing, is vital to living a life of wholeness, balance, and contentment. In simple terms, an emotional health definition is one that includes resilience or getting up when life knocks you down. There is a difference between mental health and emotional health. Emotional health is more focused on identifying, expressing, and managing feelings like anger, happiness, frustration, or powerlessness, while mental health is usually associated with illnesses such as schizophrenia and mood disorders.
Stressors
There are two types of stress: acute and chronic. Acute stress is immediate and sudden, while chronic stress is ongoing. We’ll address each type in more detail below.
Acute Stress
Acute stress is short-term stress caused by sudden stressors, such as arguments or job interviews. Our bodies are typically good at dealing with this type of stress, but we should try to reduce the impact it has. When faced with acute stressor, your emotional brain reacts faster to stimuli than your rational brain does. As a result, it will often respond to a sudden stressful situation with a “Fight, Flight, or Freeze” reaction before your rational brain has had a chance to evaluate the situation.
Chronic Stress
Chronic stress is stress that one has learned to live with over an extended period. This type of stress can cause physical health problems, such as a lower immune system and chronic fatigue, as well as mental health problems such as depression and anxiety. This is a crucial point differentiating between acute and chronic stress.
Chronic stress can arise from living in a difficult circumstance (such as long-term unemployment or chronic back pain). It can also come from dealing with difficult people for a long time (such as an emotionally abusive family member or an unpredictable and negative boss). Often, though, chronic stress comes from within.
Stress is nothing new to radiology professionals. A whole host of stressors come as part and parcel of the job, and are increased in times of difficulty or crisis. These stressors include staffing shortages, physical injuries, hospital violence, and diverse types of fatigue. While stressors are unique and personal to everyone, they can also be applied to all radiology professionals and can correlate with health deficiencies.
The gist: We’re pretty good at handling acute stress, but chronic stress can have severe effects on a person’s physical and mental health and must be identified and addressed for the health of the RT and for the safety of patients they image.
COVID-19’s Role in Radiologic Technologist Burnout
Healthcare workers (HCWs) during the COVID-19 pandemic experience numerous psychological problems, including stress and anxiety. These can affect sleep quality and predispose healthcare workers to insomnia. The results of a recent study conducted from January 2020 to January 2021 showed a relatively high prevalence of insomnia among HCWs during the COVID-19 pandemic. As insomnia can be associated with other psychological problems, policymakers and health managers should regularly screen healthcare workers for psychological disorders, as well as for a tendency for suicide. In addition, treating insomnia can reduce the incidence of these psychological disorders.
This is not to mention stress caused by staffing shortages, hospitals filled to capacity, moral outrage at those who refuse vaccination and then end up in a hospital bed with COVID, trauma from death, worry and fear of contracting the virus, and other stressors. And the protracted nature of this pandemic, of the stressors to with rad techs and other HCWs are exposed, has driven an uptick in rad tech burnout.
The gist: The prolonged exposure to pandemic-related stressors such as short staffing, longer shifts and reduced sleep, trauma, fear, and anxiety have increased the rate at which rad techs are “burning out.”
Gender Differences
A person’s gender significantly shapes their perceptions of risk and their coping strategies for stress and anxiety. A recent study in Pakistan showed perceived fear and trust to vary significantly between men and women, as well as notable differences in the coping mechanisms used by men and women. In the study, women perceived risks to be greater, more often and readily complied government guidelines, and showed better coping than males in response to COVID-19. This suggests that RTs of different genders may differ in recognizing risk, may experience stress differently on the job, and may need different levels of support when working to develop a toolbox of coping mechanisms to maintain their emotional health.
Coping Mechanisms
Below we provide a few things RTs can try to manage symptoms of stress and fatigue and try to prevent burnout and maintain good emotional health. For a more in-depth look at coping strategies and a list of helpful resources for managing stress, anxiety, and pandemic-related stress, check out our article: Coping with Stress During the COVID-19 Pandemic: Suggestions for Rad Techs.
- Meditation – the practice where an individual uses a technique such as mindfulness, or focusing the mind on a particular object, thought, or activity to train attention and awareness, and achieve a mentally clear and emotionally calm and stable state.
-
- Physical Exercise – exercise in almost any form can act as a stress reliever by increasing overall health and sense of well-being. Physical activity may help bump up the production of endorphins, the brain’s feel-good neurotransmitters and can reduce the negative effects of stress. Exercise can also has positive effects on the cardiovascular, digestive, and immune systems by helping protect the body from harmful effects of stress. Exercising regularly, though sometimes difficult for overworked and stressed-out individuals, can actually increase self-confidence, improve mood, and lower symptoms of mild depression and anxiety. Exercise can also improve sleep, which is often disrupted by stress, depression, and anxiety. As we mentioned above, poor sleep can lead to negative psychological effects and poor performance on the job.
- Music as a coping strategy – music can have a powerful effect on your body and your emotions and is effective in stress management. Fast music can make you more alert and help with concentration; upbeat music can trigger more optimistic and positive feelings about life; and music with a slow tempo being soothing and assist in stress-relief, as it can quiet your mind and relax your muscles.
- Artistic expression gives us the chance to communicate our thoughts, feelings, hopes, dreams, fears, and any other number of internal parts of ourselves to others. And expressing our inner selves can be beneficial for our physical and mental health by taking our attention away from our present stressors and providing necessary downtime.
The gist: Staying physically active for at least 30 minutes a day can help to improve your overall emotional health. The exercise does not need to be overly tough or intense, just going for a walk or dancing around your house can help. Remember, meditation helps you to notice your thoughts and emotions, which is key to emotional wellness.
Final Thoughts
Stress, fatigue, and burnout remains an inherent part of working in the healthcare field. While these last few years have enhanced the stress accompanying this work, learning to cope to alleviate fatigue and burnout is more important now than ever. Sources of burnout are work overload, social conflicts, and lack of resources. A major consequence of stress is burnout that may cause an individual to leave their profession. COVID-19 has brought this to the forefront, though it has been long overdue for the profession to address knowledge about and skills sets for maintaining emotional health, since the health of the RT has a direct impact on the quality of patient care he or she can provide.
References
- Ballinger, J.M, Comello, R.J., & Vealé, B. (2008). Stressors that negatively affect the health of radiology professionals. Journal of Medical Imaging and Radiation Sciences, 39(1), 11-15. [Link]
- Berg, S. (2021, May 25). This first-aid kit will help you treat stress in health care. American Medical Association. [Link]
- Brown, G. (2018, August 14). Difference between mental health and emotional health. Difference Between. [Link]
- Cohen, T., & Legg, J. (2019). Emotional well-being and stress among radiologic science students. Radiologic Technology, 90(5), 450–458.
- De Hert, S. (2020). Burnout in Healthcare Workers: Prevalence, Impact and Preventative Strategies. Local and Regional Anesthesia, 13, 171–183. [Link]
- Freudenberger, H.J. (1982) Counseling and dynamics: treating the end-stage person. In J.W. Jones (Ed.), The burnout syndrome. Park Ridge III: London House Press.
- Harris, M., Wilson, J. C., Holmes, S., & Radford, D. R. (2017). Perceived stress and well-being among dental hygiene and dental therapy students. British Dental Journal, 222(2), 101–106. [Link]
- Howlett, M., et al. (2015). Burnout in emergency department healthcare professionals is associated with coping style: a cross-sectional survey. Emergency Medicine Journal, 32(9), 722–727. [Link]
- Liu, S., et al. (2021). Gender differences in mental health problems of healthcare workers during the coronavirus disease 2019 outbreak. Journal of Psychiatric Research, 137, 393–400. [Link]
- Mayo Clinic. (2020, August 18). Exercise and stress: Get moving to manage stress. [Link]
- Occupational Safety and Health Administration. (n.d.). Long work hours, extended or irregular shifts, and worker fatigue. [Link]
- Ramirez, L. (2021, July 3). How to relieve stress through artistic expression. Chamber of Thoughts. [Link]
- Rana, I. A., Bhatti, S. S., Aslam, A. B., Jamshed, A., Ahmad, J., & Shah, A. A. (2021). COVID-19 risk perception and coping mechanisms: Does gender make a difference?. International Journal of Disaster Risk Reduction, 55, 102096. [Link]
- Reingold L. (2015). Evaluation of stress and a stress-reduction program among radiologic technologists. Radiologic Technology, 87(2), 150–162.
- Sahebi, A., Abdi, K., Moayedi, S., Torres, M., & Golitaleb, M. (2021). The prevalence of insomnia among health care workers amid the COVID-19 pandemic: An umbrella review of meta-analyses. Journal of Psychosomatic Research, 149, 110597. [Link]
- Shaw, E. (2021, June 29). Acute vs chronic stress: 2 types of stress explained. Short Form. [Link]
- Smith, C. S., Folkard, S., Tucker, P., & Evans, M. S. (2011). Work schedules, health, and safety. In J. C. Quick & L. E. Tetrick (Eds.), Handbook of Occupational Health Psychology (pp. 185–204). American Psychological Association.
- Terp, U., Bisholt, B., & Hjärthag, F. (2019). Not just tools to handle it: A qualitative study of nursing students’ experiences from participating in a cognitive behavioral stress management intervention. Health Education & Behavior, 46(6), 922–929. [Link]
- University of Nevada, Reno. (n.d.), Releasing stress through the power of music. [Link]
- Ya’qoub, L., Elgendy, I. Y., & Pepine, C. J. (2021). Sex and gender differences in COVID-19: More to be learned!. American Heart Journal Plus: Cardiology Research and Practice, 3, 100011. [Link]
- Yang, Y., Peng, F., Wang, R., Yange, M., Guan, K., Jiang, T., Xu, G., Sun, J., & Chang, C. (2020). The deadly coronaviruses: The 2003 SARS pandemic and the 2020 novel coronavirus epidemic in China. Journal of Autoimmunity, 109, 102434. [Link]
- Yee, K.M. (2020, April 4). Is radiology prepared for a post-COVID-19 imaging surge? Aunt Minnie. [Link]
Disclaimer: The information provided on this website is intended to provide useful information to radiologic technologists. This information should not replace information provided by state, federal, or professional regulatory and authoritative bodies in the radiological technology industry. While Medical Professionals strives to always provide up-to-date and accurate information, laws, regulations, statutes, rules, and requirements may vary from one state to another and may change. Use of this information is entirely voluntary, and users should always refer to official regulatory bodies before acting on information. Users assume the entire risk as to the results of using the information provided, and in no event shall Medical Professionals be held liable for any direct, consequential, incidental or indirect damages suffered in the course of using the information provided. Medical Professionals hereby disclaims any responsibility for the consequences of any action(s) taken by any user as a result of using the information provided. Users hereby agree not to take action against, or seek to hold, or hold liable, Medical Professionals for the user’s use of the information provided.



